Clinical evidence of gum infection predicts undiagnosed diabetes
Periodontitis has been identified as the sixth complication of diabetes. Advanced glycation end-products, altered lipid mechanisms, oxidative stress, and systemically elevated cytokine levels in patients with diabetes and periodontitis suggest that dental and medical care providers should coordinate therapies.
Inflammation of the Periodontium
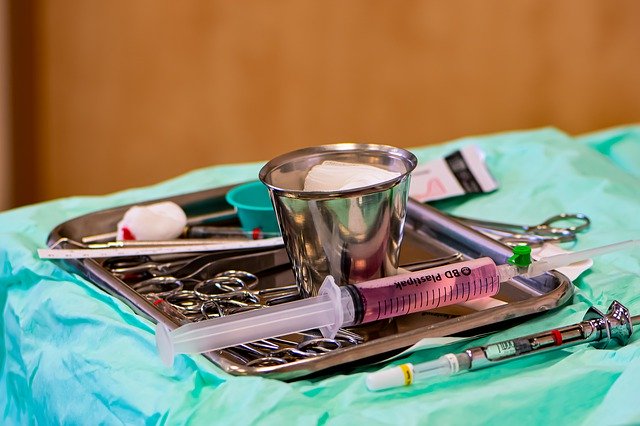
Periodontitis is a chronic inflammatory disease of the mouth that involves the gingiva (gum tissues), teeth, and supporting bone. Periodontitis is clinically defined as the loss of connective tissue attachment to the teeth and alveolar bone loss. If periodontitis is left untreated, the involved teeth will exfoliate.
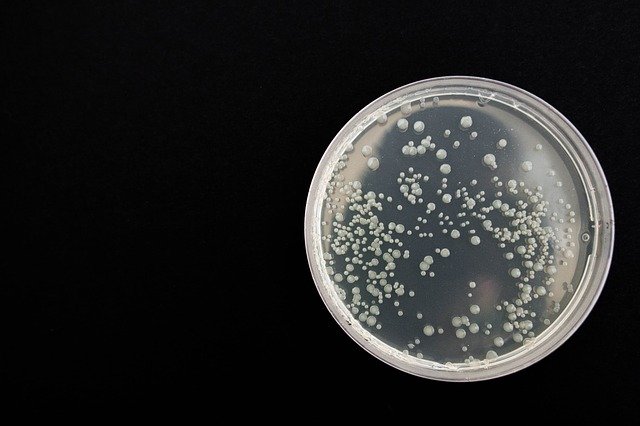
In many cases, periodontitis is the second stage of an inflammatory process that begins with gingivitis. From a clinical perspective, gingivitis presents with swollen tissues and increased redness but with no loss of connective tissue attachment between root surfaces and bone. The inflammatory cell infiltrate in gingivitis is dominated by a polymorphonuclear neutrophil infiltrate (acute inflammation), whereas the histopathology of periodontitis is dominated by a plasma cell infiltrate (chronic inflammation).1
The clinical signs of periodontitis include swelling, redness and bleeding from the gums, spacing between teeth, loose teeth, and exposure of root surfaces through loss of bone around the teeth.
Continue reading